TORONTO’S PREMIER PLASTIC SURGEON
Dr. Stephanie Power
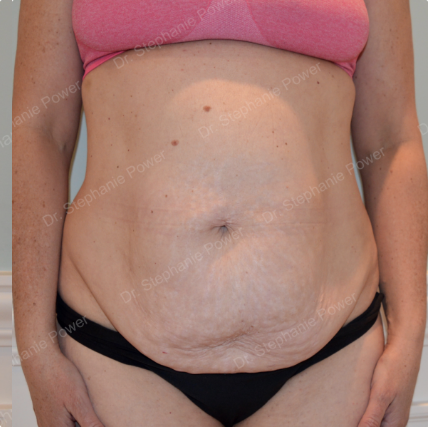
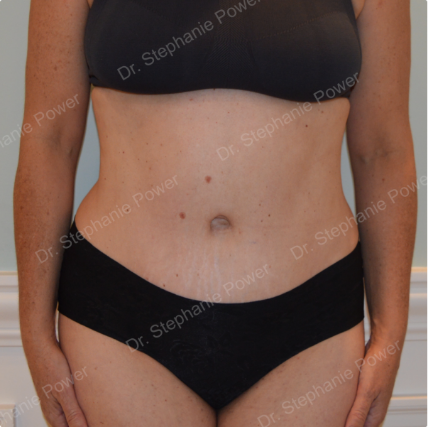
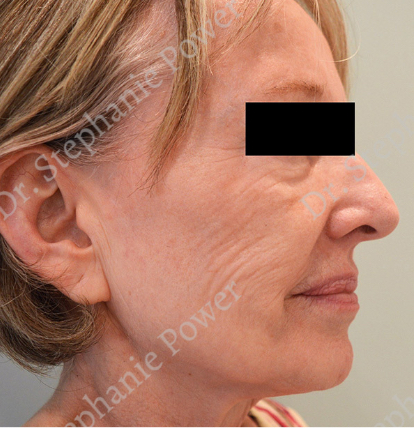
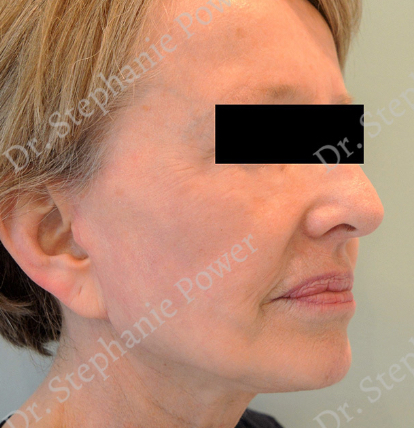
Dr. Power is one of only a few female cosmetic surgeons in Toronto, bringing a feminine and fresh perspective to plastic surgery. Her practice focuses on the female body and facial aging. Dr. Power understands the sensitive nature of cosmetic surgery and is attuned to patients’ concerns, striving to make all patients feel comfortable.
MEET DR. POWER